26 Feb Art of Re-entry: Practical Strategies for When Your Antegrade Wire Lands Subintimal
The moment your antegrade wire slips into the subintimal space is one of the most common and challenging junctions in chronic total occlusion work. This is where technique, planning, and calm decision making separate a controlled re-entry from a prolonged, futile battle. The goal is simple: get back into the true lumen safely, preserve side branches, and avoid making the distal vessel unrecoverable.
Table of Contents
- Why re-entry planning matters
- Use imaging to choose and protect the re-entry zone
- Initial maneuvers when you’re subintimal
- Stingray re-entry: step-by-step practical tips
- When re-entry is difficult: read the anatomy and correct the physiology
- Facilitated ADR: protecting the true lumen during re-entry
- Tip-detection re-entry with intravascular ultrasound (IVUS)
- When to stop and switch strategy
- Practical checklist for re-entry readiness
- Common pitfalls and how to avoid them
- Summary
- Frequently Asked Questions
Why re-entry planning matters
Re-entry is not an afterthought. It should be part of the plan before you even cross the proximal cap—especially when retrograde options are limited or absent. The moment the wire goes subintimal, several competing techniques become available: redirect the same wire, escalate the wire, use a parallel wire with a stiffer or escalated tip, employ a dedicated re-entry device such as Stingray, use intravascular ultrasound guided tip-detection re-entry, or convert to a retrograde approach. Each option has strengths and drawbacks.
Key concept: the first three strategies—redirection, wire escalation, and parallel wiring—can be mutually exclusive in practice. Spending a long time committed to one approach can make the others impossible because vessel clarity degrades and subintimal hematoma increases.
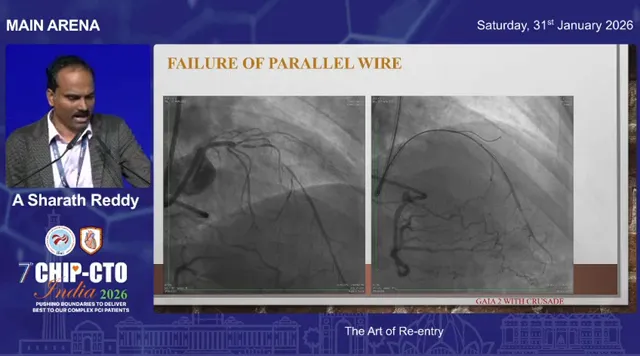
Use imaging to choose and protect the re-entry zone
Computed tomography angiography and careful angiographic planning are invaluable. When facing a long, calcified CTO it is essential to identify a re-entry zone where the vessel is relatively free of calcium and visible on angiography. Pick that spot and protect it from repeated knuckle passes and aggressive subintimal maneuvers.
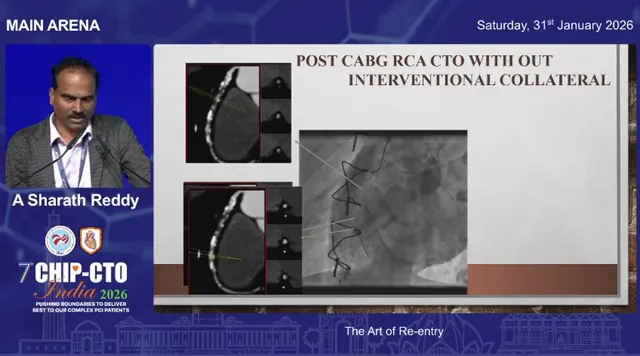
Ask the right questions before you commit: Where will I attempt re-entry? What support will I need? What is my planned dissection or crossing strategy? If the wire has already entered the subintimal space because of an antegrade collision, refine the answers: how will I protect my re-entry zone from intramural hematoma and what re-entry method will I use?
Initial maneuvers when you’re subintimal
Before deploying a re-entry tool, strengthen support and prepare the pathway.
- Anchor and trap technique: trap the microcatheter by inflating a balloon proximally to get additional support for device exchanges and advancement.
- Create space for the re-entry device: a 1.0 mm balloon inflation can help dilate the subintimal plane. Alternatively advance a supportive microcatheter or Corsair-type catheter over an exchange wire to create a track for the re-entry catheter.
- Use an exchange wire: once the track is prepared, exchange to a stiffer support wire to deliver the Stingray or other re-entry platform.
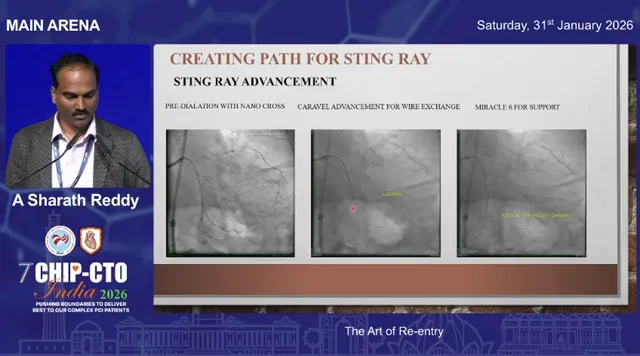
Stingray re-entry: step-by-step practical tips
The Stingray system is a powerful tool for controlled re-entry when a suitable angiographic re-entry zone exists. The technique has pitfalls; following a systematic approach increases the chance of success.
- Choose the re-entry zone: preferably where the vessel lumen is clearly seen and calcium burden is low on cross-section imaging.
- Enhance support: place an anchor wire into a side branch or distal vessel to enhance pushability for Stingray delivery.
- Create a track: dilate the subintimal space with a small balloon or advance a microcatheter and exchange for a stiff wire. Then advance the Stingray catheter along that stiff wire to the planned re-entry spot.
- Obtain the correct angiographic view: recognize that there are different orientations of the Stingray balloon. The “side” view is not the right view for re-entry. Make sure you obtain the optimal view (face-on) so that the Stingray exits align toward the true lumen.
- Contrast injection: inject contrast with the Stingray in place to map where the true lumen lies relative to the Stingray exits.
- Trial and error with the Stingray wire: any of the Stingray exits can lead to the true lumen. Advance the Stingray wire through the chosen exit; if you enter the true lumen, exchange to a workhorse wire and proceed.
Practical note: There is no single “magic exit” on the Stingray that always points to the true lumen. Re-entry may require a few attempts at different exits until the wire enters the lumen. Swapping to a pilot or other soft workhorse wire after re-entry will make device delivery easier.
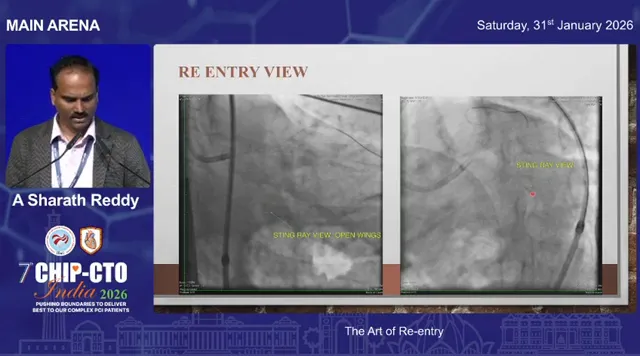
When re-entry is difficult: read the anatomy and correct the physiology
As the procedure progresses the subintimal space can expand and subintimal hematoma (SIH) can push the true lumen away from your re-entry device. Increased SIH is the most common reason why a seemingly straightforward re-entry becomes impossible.
Options when re-entry becomes challenging:
- Reduce the hematoma: techniques to decompress the subintimal space can bring the true lumen closer to the re-entry device. This may mean balloon fenestration, aspiration, or controlled fenestration maneuvers designed to change the anatomy of the subintimal space and reduce the compressive effect on the true lumen.
- Move the Stingray: bobbing or sliding the Stingray to a nearby spot where the true lumen is closer can convert a failed re-entry attempt into a successful one. Make small adjustments rather than large repositioning to minimize additional trauma.
- Enhanced support and parallel strategies: place a wire in a side branch to anchor and then re-attempt re-entry with a supported Stingray catheter over a stiff wire.
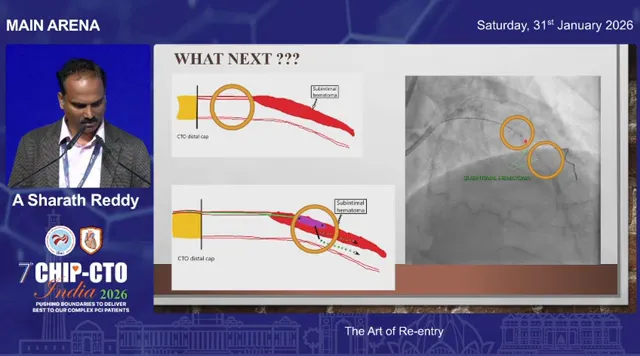
Facilitated ADR: protecting the true lumen during re-entry
Facilitated antegrade dissection and re-entry is particularly useful in post-CABG patients or when the distal vessel is accessible via a retrograde channel, even if that channel is not ideal for crossing retrogradely.
The facilitated ADR sequence can look like this:
- Perform antegrade dissection intentionally and advance into the subintimal plane.
- Go retrograde with a wire into the distal true lumen or PDA via available collaterals or a graft channel.
- Pass a low-profile balloon retrograde and inflate it in the distal true lumen at the planned re-entry site.
- Use the inflated balloon as a protected target and direct the antegrade wire toward it. The balloon both marks the re-entry site and physically protects the distal true lumen from extended subintimal damage.
This strategy lets you extend an otherwise risky knuckle or sliding knuckle all the way close to the re-entry zone because the inflated balloon preserves the true lumen and provides a visible target for re-entry.
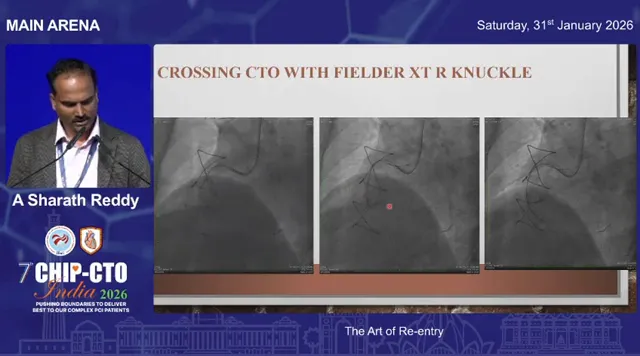
Tip-detection re-entry with intravascular ultrasound (IVUS)
When conventional angiographic methods fail, intravascular ultrasound becomes a reliable option for tip-detection re-entry. Under IVUS guidance you can directly visualize the relationship between the catheter tip, the subintimal plane, and the true lumen. Use IVUS to:
- identify the true lumen in real time;
- guide precise orientation of the re-entry wire;
- confirm wire position before committing to ballooning or stenting.
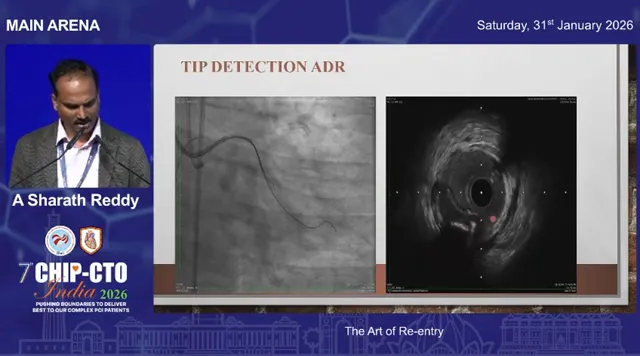
IVUS-guided tip detection reduces the guesswork. In large subintimal spaces it can be the difference between a lengthy failed attempt and a controlled, successful re-entry. In some cases, because the subintimal space is huge and the distal vessel disease is diffuse, the final strategy may simply be to perform an “investment” with balloon-only therapy and stop—preserving distal vessels for future options.
When to stop and switch strategy
Not every CTO is a candidate for aggressive re-entry. Diffuse distal disease, poor distal targets, and cases where repeated re-entry attempts enlarge the subintimal hematoma to the point of jeopardizing the distal vessel are indications to pause and reconsider. Options include:
- Investment strategy: perform limited ballooning to restore some flow and abort the intense re-entry attempt. This preserves the distal bed for later intervention.
- Staging: come back later after the vessel has healed or after planning retrograde options.
- Change approach: consider retrograde crossing, surgical referral, or hybrid approaches depending on collateral availability and patient factors.
Practical checklist for re-entry readiness
Before you commit to a re-entry attempt, run through this checklist:
- Re-entry zone identified: confirmed by CTA or angiography and free of heavy calcium on cross-section.
- Support plan in place: anchor wire or side-branch wire positioned if needed.
- Space creation method: 1.0 mm balloon or microcatheter strategy ready for Stingray delivery.
- Imaging tools available: IVUS or other imaging for tip-detection if required.
- Backup strategies: have a parallel wire, retrograde plan, or investment plan ready if re-entry fails.
Common pitfalls and how to avoid them
- Over-commitment to one technique: avoid hanging on to a single method for too long. If you spend a lot of time knuckling or redirecting without progress, your angiographic clarity may degrade and options narrow.
- Ignoring imaging: skip CTA and IVUS at your peril. They reveal target zones and calcium burden that fluoroscopy alone cannot.
- Poor orientation of Stingray: ensure the correct angiographic projection. The wrong view looks fine but can mislead the operator about exit alignment.
- Failure to reduce subintimal hematoma: when the lumen is compressed by SIH, strategy should pivot to decompression techniques prior to re-attempt.
Summary
Re-entry is a skill and a decision-making process. When your antegrade wire lies in the subintimal plane, you have multiple tools and tactics: redirect the wire, escalate, use a parallel wire, deploy Stingray, use IVUS-guided tip detection, or go retrograde. Each choice requires preparation—identify and protect the re-entry zone, ensure adequate support, create the pathway for the device, and choose the correct views during re-entry.
Remember that the first three options can negate each other if pursued too long. Be ready to change strategy, reduce subintimal hematoma promptly, and use facilitated ADR or IVUS if conventional attempts fail. Finally, be willing to stop and invest when the anatomy or patient safety dictates.
Frequently Asked Questions
What are the immediate options when my antegrade wire becomes subintimal?
The main options are redirect the same wire, escalate to a stiffer or different tip wire, use a parallel wire strategy, use a dedicated re-entry device such as Stingray, perform IVUS-guided tip-detection re-entry, or change to a retrograde approach. Choice depends on anatomy, available collaterals, and the operator’s plan.
How do I pick and protect a re-entry zone?
Use CTA and angiography to identify a segment with minimal calcium and good visibility. Save that spot from repeated knuckle passes and heavy instrumentation. Anchor or trap the microcatheter proximally when necessary to preserve access to the zone.
When should I use Stingray versus IVUS-guided re-entry?
Stingray is effective when you have an angiographically visible, non-calcified re-entry zone and can create a track for the device. IVUS is preferred when the anatomy is ambiguous or when subintimal hematoma has distorted the lumen; it provides direct visualization and precise tip detection for re-entry.
What are the signs that subintimal hematoma is preventing re-entry?
A buckling or coiling wire on attempted re-entry, persistent failure across multiple exits, and progressive loss of angiographic lumen visibility are classic signs. In this setting, decompression or fenestration to reduce the hematoma is often required.
How does facilitated ADR with a balloon work?
Facilitated ADR uses a retrograde balloon placed and inflated in the distal true lumen to mark and protect the re-entry site. The antegrade wire is directed toward the inflated balloon; the balloon preserves the distal lumen and serves as a visible, physical target for re-entry.
When is it better to stop and use an investment strategy?
If repeated attempts create large subintimal spaces, distal target disease is diffuse, or no viable retrograde options exist, a controlled stop with balloon-only therapy (investment) preserves distal vessels and allows future staged strategies. Patient safety and distal vessel preservation should guide this decision.


No Comments